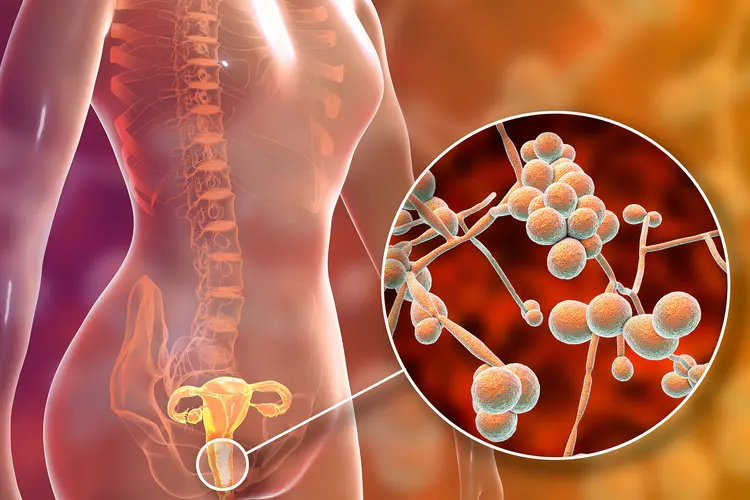
What Is a Vaginal Yeast Infection?
What Is a Vaginal Yeast Infection? A vaginal yeast infection is a fungal infection that occurs in the vaginal area and is usually caused by a type of fungus called Candida albicans. This condition is quite common among women, and many are likely to experience this type of infection at some point in their lives. Vaginal yeast infections are often influenced by factors such as excessive moisture, hormonal imbalances, and antibiotic use. The infection develops when the natural balance of the vaginal flora is disrupted and presents with various symptoms. The discomfort caused by a vaginal yeast infection is typically associated with itching, burning, and abnormal discharge. These symptoms can negatively affect daily life and may require treatment. Additionally, vaginal yeast infections are linked to improper antibiotic use or a weakened immune system. Therefore, it is important to consult a healthcare professional if such symptoms occur. What Are the Symptoms of a Vaginal Yeast Infection? Vaginal yeast infections are a common health issue among women. These infections are typically caused by a fungus known as Candida and present with specific symptoms. The most common symptoms include: Itching and discomfort Increased vaginal discharge, usually white and thick (cottage cheese-like) Burning or pain during urination Pain during sexual intercourse Redness or swelling of the outer vaginal area The presence of these symptoms may indicate a vaginal yeast infection. However, a physician should always be consulted for an accurate diagnosis. Identifying the exact cause of the infection is essential for proper treatment. What Causes a Vaginal Yeast Infection? A vaginal yeast infection usually occurs due to the overgrowth of Candida albicans. Normally present in the vagina, this fungus begins to multiply when the immune system weakens or when the pH balance is disrupted. Several factors may contribute to this condition. Antibiotic use can reduce beneficial bacteria in the vagina, creating an environment for fungal overgrowth. Hormonal changes, pregnancy, and birth control pills may also trigger vaginal yeast infections. Certain health conditions, such as diabetes, can weaken the immune system and increase susceptibility to infections. Stress, poor nutrition, and inadequate hygiene are also contributing factors. Since many lifestyle and health factors play a role, maintaining a healthy lifestyle and taking preventive measures are important for protecting vaginal health. How Is a Vaginal Yeast Infection Diagnosed? Diagnosis begins with evaluating the patient’s complaints and performing a physical examination. The doctor listens carefully to symptoms and conducts a vaginal exam. A key part of diagnosis involves laboratory analysis of vaginal discharge to confirm the presence of a fungal infection. If a yeast infection is detected, appropriate treatment options are determined. In some cases, a vaginal culture test may be performed to identify the specific fungal type and select the most effective treatment. Additional tests may be required to rule out other infections. Accurate diagnosis ensures the correct treatment process is initiated. Treatment Methods and Medications for Vaginal Yeast Infections A vaginal yeast infection can be managed with various treatment options depending on the severity and individual health condition. Common treatments include antifungal medications available as creams, oral tablets, or vaginal suppositories. These help stop fungal growth and relieve symptoms. Medications containing clotrimazole or miconazole are frequently used. Patients are also advised to maintain good genital hygiene, prefer cotton underwear instead of synthetic fabrics, and follow a balanced diet to help maintain vaginal flora balance. In some cases, natural supportive methods may be considered. Probiotic supplements and fermented foods like yogurt may help restore healthy vaginal flora. However, consulting a healthcare professional before starting any treatment is essential. What Helps with a Vaginal Yeast Infection? Certain natural and home-based methods may help relieve symptoms, but they do not replace medical treatment. Some suggestions include: Probiotics: Yogurt or probiotic supplements may help balance vaginal flora and prevent recurrence. Natural Oils: Tea tree oil and lavender oil have antifungal properties that may help reduce irritation. Apple Cider Vinegar: Adding it to bathwater may help restore vaginal pH balance, but direct application should be avoided. Garlic: Known for antifungal properties, it can be consumed as part of the diet or as a supplement. Good Hygiene: Keeping the vaginal area dry and clean helps prevent infections. If symptoms persist or worsen, consult a specialist. How Long Does a Vaginal Yeast Infection Last? Although treatable, recovery time varies from person to person. Symptoms often improve quickly after starting treatment, but full recovery may take several days to a few weeks. Lifestyle adjustments, such as proper hygiene, avoiding tight clothing, and choosing cotton underwear, can support faster recovery. In individuals with weakened immune systems or recurrent infections, healing may take longer. If symptoms persist or frequently recur, seeking medical advice is important. When treated properly, vaginal yeast infections typically resolve quickly, though individual factors may influence recovery time. Frequently Asked Questions What is a vaginal yeast infection?It is the overgrowth of a Candida fungus in the vagina, causing infection. What are the symptoms?Symptoms include itching, burning, changes in discharge, and vaginal discomfort. What causes vaginal yeast infections?Causes include antibiotic use, hormonal changes, weakened immunity, and certain dietary or health factors. How is it treated?Treatment usually involves antifungal creams or oral medications. How can it be prevented?Maintaining hygiene, avoiding synthetic underwear, and following a healthy diet are important preventive measures. Who is more likely to experience it?Pregnant women, individuals with diabetes, and those with weakened immune systems are more susceptible. What happens if it is not treated?Untreated infections may worsen and potentially lead to more serious complications such as pelvic infections.