What Is Asherman Syndrome?
What Is Asherman Syndrome?
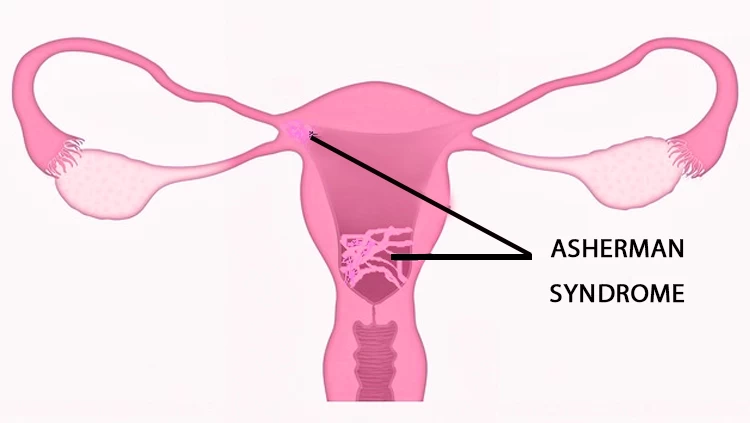
Asherman Syndrome is a condition that causes scar tissue (adhesions) to form inside the uterus. This scar tissue can cause the walls of the uterus to stick together, affecting a woman’s ability to menstruate normally and become pregnant. It usually develops after postpartum complications, surgical procedures, or intrauterine interventions. The condition may present with symptoms such as absence of menstruation, menstrual irregularities, or infertility.
Asherman Syndrome often requires surgical treatment; however, if diagnosed and treated early—before adhesions fully develop—complications can be prevented. More detailed information about diagnosis and treatment options should be obtained by consulting specialist physicians.
Symptoms of Asherman Syndrome and Diagnostic Methods
Asherman Syndrome is characterized by adhesions and scar tissue within the uterus. Symptoms may include menstrual irregularities, painful periods, or absence of menstruation. Some women may experience difficulty becoming pregnant due to Asherman Syndrome. The condition often develops after pelvic surgery, intrauterine procedures, or postpartum bleeding.
The diagnostic process is supported by imaging techniques in addition to evaluating the patient’s symptoms. Hysteroscopy is one of the most effective methods for diagnosing this condition. During this procedure, a hysteroscope is used to directly visualize the inside of the uterus and detect adhesions.
Other imaging methods such as X-ray or ultrasound may also be used; however, hysteroscopy allows for a more comprehensive evaluation of Asherman Syndrome. Recognizing symptoms and using appropriate diagnostic methods are critical for determining the severity of the condition and planning suitable treatment.
Early diagnosis is important. Therefore, women experiencing menstrual irregularities or difficulty conceiving should consult a healthcare professional for proper evaluation.
Causes and Risk Factors of Asherman Syndrome
Asherman Syndrome typically occurs as a result of scar tissue formation in the inner uterine wall. This scar tissue may develop due to various reasons. The primary causes include previous uterine surgeries, postpartum complications, or infections. In particular, dilation and curettage (D&C) procedures are significant triggering factors.
Another risk factor includes women who have previously experienced abnormal conditions within the uterus. Any trauma, infection, or surgical intervention may increase the risk of developing Asherman Syndrome. Additionally, hormonal imbalances in some women may influence the formation of scar tissue.
Genetic predisposition and immune system-related problems are also considered potential risk factors. These conditions may trigger inflammatory processes within the uterus, increasing scar formation.
A woman’s past experiences related to sexual and reproductive health may also be important determinants. Therefore, regular health check-ups are recommended, especially for those with known risk factors.
What Are the Treatment Options for Asherman Syndrome?
Treatment for Asherman Syndrome varies depending on the severity of the condition and the patient’s overall health. The first step is a detailed evaluation of the patient’s condition. In most cases, adhesions inside the uterus are removed through a procedure called hysteroscopy. This allows the doctor to directly visualize the uterine cavity and remove abnormal tissue.
In some cases, additional treatment methods may be required after hysteroscopic surgery. For example, hormone therapy may be used to reduce the risk of re-adhesion within the uterus. Regular follow-up examinations are also very important after treatment.
Alternative approaches may also be considered. Some women may benefit from natural methods and lifestyle changes; however, it is important to note that the effectiveness of these methods is not scientifically proven.
Treatment options for Asherman Syndrome vary, and patients should work closely with their doctors throughout the process.
Success Stories Related to Asherman Syndrome
Although Asherman Syndrome can be a challenging experience, many women have overcome it and gone on to have successful pregnancies. These success stories serve as a source of hope for those facing the condition.
Many women, after receiving a diagnosis, pursued appropriate treatments and ultimately experienced the joy of becoming mothers. Hysteroscopic surgery, which removes uterine adhesions, has enabled many women to conceive again. Here are some inspiring examples:
Ayşe’s Story: Diagnosed with Asherman Syndrome at age 35, Ayşe conceived naturally after hysteroscopic surgery and now has a healthy baby.
Zeynep’s Experience: After two consecutive miscarriages, 28-year-old Zeynep was diagnosed with Asherman Syndrome. Following treatment, she conceived through IVF and gave birth to twins.
Fatma’s Success Story: At age 40, Fatma had tried many treatments without success due to Asherman Syndrome. After surgery, she finally received the joyful news that she was pregnant.
These stories demonstrate that with proper treatment, the challenges of Asherman Syndrome can be overcome. Support groups and shared experiences on social media can provide encouragement for women facing similar journeys.
Ways to Increase Pregnancy Chances with Asherman Syndrome
For individuals diagnosed with Asherman Syndrome, the path to pregnancy may involve certain challenges. However, several methods and treatments may help increase the chances of conception:
Medical Treatment: Doctors may recommend hormone therapy to improve the uterine environment and enhance the likelihood of pregnancy.
Surgical Intervention: Removing intrauterine adhesions surgically is one of the most effective ways to improve pregnancy chances. Hysteroscopy is commonly preferred.
Intrauterine Devices: After surgery, temporary devices may be placed inside the uterus to help prevent re-adhesion and maintain a suitable environment for pregnancy.
Nutrition and Lifestyle Changes: A healthy diet and regular exercise can improve overall health and potentially increase fertility. Anti-inflammatory foods may help maintain hormonal balance.
Psychological Support: Coping with Asherman Syndrome can be emotionally challenging. Psychological support can reduce stress and positively influence fertility.
Consulting a specialist is essential to determine the most appropriate individualized approach.
Coping with Asherman Syndrome
Coping with Asherman Syndrome can be physically and emotionally demanding. Adopting effective coping strategies is important.
Open communication with family and friends can provide emotional support and reduce feelings of isolation. Support groups can also be beneficial, allowing individuals to share experiences with others facing similar challenges.
Stress management techniques such as meditation, yoga, and deep breathing exercises may help strengthen mental health and improve overall quality of life.
Regular check-ups with a healthcare professional are crucial for monitoring both physical and mental well-being. Following professional guidance helps ensure proper treatment and overall health management.
Frequently Asked Questions
What is Asherman Syndrome?
Asherman Syndrome is a condition characterized by adhesions and scar tissue formation inside the uterus, often occurring after pregnancy loss or surgical procedures.
What are the symptoms of Asherman Syndrome?
Symptoms may include irregular menstrual cycles, reduced or absent menstrual bleeding, painful periods, and infertility.
What causes this syndrome?
It is usually caused by uterine surgical procedures, infections, or postoperative complications.
How is Asherman Syndrome diagnosed?
Diagnosis is typically made through medical history evaluation, ultrasound imaging, hysteroscopy, and in some cases, biopsy.
Can Asherman Syndrome be treated?
Yes. Treatment usually involves hysteroscopic removal of adhesions and may be supported by hormone therapy.
What are the risk factors?
Risk factors include previous uterine surgeries, recurrent miscarriages, uterine infections, and certain medical conditions.
Is it possible to prevent this syndrome?
While it may not be completely preventable, minimizing unnecessary surgical procedures and ensuring proper treatment and follow-up can help reduce the risk.
